Welcome to Our Training Page!
The University of British Columbia Pediatric Critical Care Training Program is fully accredited by the Royal College of Physicians and Surgeons of Canada. The program is based at British Columbia’s Children’s Hospital, which is the only tertiary care pediatric facility in BC, serving a population of approximately 4,500,000. Further details regarding the hospital can be viewed under the “Hospital Information” tab.
Canadian trainees who have completed training in a Royal College approved program including Anesthesiology, Pediatric Cardiac Surgery, Emergency Medicine, Pediatric General Surgery or in their 4th year of Pediatrics are eligible for enrolment in our Pediatric Critical Care Subspecialty Training Program via the Canadian Residency Matching Service. They must complete 2 years of training to achieve certification. Entry from other eligible programs will be considered on an individual basis. Critical Care Medicine is a complex discipline, requiring the trainee to acquire a large body of knowledge and skills in a relatively short two-year period. Hence, we do not offer combined training with any other programs.
Training includes a total of 26 blocks of training (13 blocks per year). The majority of that time is spent divided between the CICU and MSICU units. Time is afforded each year for a few blocks of elective including anesthesia time. Research time is provided with dedicated blocks for those who require it and longitudinal research time in order to attend to research goals weekly. Electives have been offered in NICU, cardiology, transport, palliative care, trauma, toxicology, emergency medicine, global health and adult ICU. The program is open to rotations outside of those listed if they are relevant to career goals and training.
Weekly protected academic time is scheduled to meet Royal College objectives. This includes case conferences, morbidity/mortality rounds, lectures by staff and trainees, combined rounds with cardiology and emergency medicine, and many more. These sessions are designed to facilitate learning for the trainee. Over the two year training period, residents will be exposed to the core concepts of Critical Care Medicine.
We have an active multidisciplinary simulation program that provides additional exposure to resuscitative and critical care scenarios, as well as a fully functional high fidelity Extra Corporeal Life Support (ECLS) simulation facility.
We require all of the Critical Care residents to be certified in Pediatric Advanced Life Support (PALS) and Advanced Cardiac Life Support (ACLS).
For International Applicants, please refer to the “Application Process” tab below for important information regarding categories of training.
UPDATED March 7th, 2025
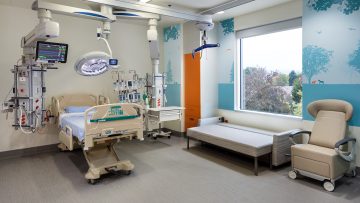
Hospital Information TECK Acute Care Centre PICU BC Children's Hospital (BCCH) provides expert care for the province's most seriously ill or injured children, including newborns and adolescents. Based in Vancouver, BCCH reaches across the province with vital health services that may not be available anywhere else in BC. We provide specialized training in pediatric health care and work with renowned researchers to achieve better health for children and youth. BCCH is affiliated with the University of British Columbia, Simon Fraser University, the Child and Family Research Institute, and other education and research institutions. The Hudson Family Pediatric Intensive Care Unit is a 28 bed facility, separated into 3 distinct pods one of which is dedicated to Cardiac Intensive Care. It is located in the state of the art Teck Acute Care Centre (TACC) which opened in 2017. Single patient rooms, state of the art monitoring and a multitude of work spaces have elevated the care provided for approximately 1200 patients annually. The unit provides quaternary care pediatric critical care including all forms of cardiac surgical interventions, advanced ventilatory strategies (HFOV/HFJV), renal replacement, and extracorporeal life support. There are numerous training opportunities in these advanced therapies. The hospital has active cardiac, renal and bone marrow transplant programs. There is a very active pediatric transport and retrieval program with ample exposure for trainees. Vancouver General Hospital (VGH) has approximately 700 acute care beds, and is the major adult tertiary referral hospital in the Province. It has a full range of programs and consulting services. It functions as the provincial Trauma Centre and is the home of a number of provincial programs (burn unit, bone marrow transplantation, solid organ transplantation, spinal cord injuries and hyperbaric medicine). Elective adult critical care medicine rotations occur at this facility. Royal Columbian Hospital (RCH) is a 400 bed acute care facility under the Fraser Health Authority and provides care to the communities of New Westminster, Coquitlam and Port Moody. RCH has a staff of 600 physicians (180 family physicians and 420 specialists) and plays an active role in the medical education of students in the department of medicine at UBC, with medical students and residents rotating through the different services at RCH. Elective trauma rotations occur at this facility.
INFORMATION ON THE APPLICATION PROCESS Canadian Residents applying to our program may submit all application forms, academic transcripts and letters of reference to the based on Canadian Resident Matching Service. Once the portal opens, applications are reviewed and short-listed applicants are invited for an on-site interview. Final selections take place as per the rules set by CaRMS. For all other applicants, applications are reviewed (see materials required below) as they are received and short-listed by the Critical Care Medicine Program Training Committee. There is rolling enrolment for each January and July start date and positions are filled as suitable candidates apply. After application materials are received, eligible candidates are offered an interview by Zoom if in-person is not possible. All those involved in the interview process complete an evaluation and these evaluations, together with the application package are considered by the Residency Program Selections Committee. Successful applicants will receive a salary determined by the Department of Pediatrics (more information about this is available from the Program Director). There are stipends for on-call hours as well as the opportunity for additional income if a trainee elects to participate in the transport retrieval roster. Apart from the salary, the Program provides financial support to allow each trainee to attend a scientific meeting once each year. If you require further information please do not hesitate to contact us. Program Administrator: WHO SHOULD APPLY To be eligible, Canadian applicants must be within one year of completing a Royal College approved program prior to initiation of subspecialty training. Acceptable training includes Pediatrics, Anesthesiology, Emergency Medicine, Pediatric General Surgery, and Pediatric Cardiac Surgery. Funding is provided by the Ministry of Health for Canadians who have finished or are in the process of finishing their base training from a Royal College of Canada approved program. Pediatric critical care training is available for foreign trainees who have current certification in their own jurisdiction in Pediatrics, Anesthesiology, or Critical Care Medicine. Candidates must meet the English language proficiency requirements** of the College of Physicians and Surgeons of British Columbia. Applications are not reviewed unless accompanied by an acceptable proof of language examination as set out by the BC College of Physicians and Surgeons. There are no exceptions to this rule. Training is available for 1 or 2 years. Applications from foreign trainees must include all of the following items to be considered: APPLICATION FORM FOR FOREIGN TRAINEESPlease download the document below to apply to pediatric critical care medicine. FORM-Application-for-Approval-of-Appointment-of-Postgraduate-Fellow ROLES AND KEY COMPETENCIES IN PEDIATRIC CRITICAL CARE MEDICINEDEFINITIONPediatric critical care medicine is a multidisciplinary field concerned with infants, children and adolescents who have sustained, or are at risk of sustaining life threatening, single or multiple organ system failure due to disease or injury. Pediatric critical care medicine seeks to provide for the needs of these patients through immediate and continuous observation and intervention so as to restore health and prevent complications. A specialist in pediatric critical care medicine is a physician or surgeon who is competent in all aspects of recognizing and managing acutely ill pediatric patients with single or multiple organ system failure requiring ongoing monitoring and support.GOALSThe rapidly expanding body of knowledge regarding the treatment of the critically ill, the continuing introduction of new technology for life support, and more complex societal issues (legal, moral, ethical) have created a need for specialists trained in the recognition and management of this patient subset. To develop such specialists individual residency programs must focus on the knowledge, skills, and attitudes pertinent to the expected roles and competencies of the pediatric critical care medicine specialist.Residents training within the unique interactive environment in which the critically ill are managed must respect the rights of the patient and family and acknowledge the importance of age, gender, culture, and ethnicity.PEDIATRIC CRITICAL CARE MEDICINE COMPETENCIESThe Royal College of Canada objectives of training for Pediatric Critical Care Medicine can be viewed here. ROTATION SPECIFIC GOALS & OBJECTIVESFollow the links below to view rotation specific goals and objectives.PICU rotation goals and objectives
EVALUATIONS Please follow the link to One45 Software and log on to view or post your evaluations. RESIDENT STAFF EVALUATION AND APPEALS POLICY, FACULTY OF MEDICINE, UNIVERSITY OF BRITISH COLUMBIA This document outlines the appeal processes for resident staff in the Faculty of Medicine at the University of British Columbia in regards to evaluation and dismissal procedure. DEFINITIONS: In this document the following definitions are used: "Resident staff" means resident or fellow in the singular or plural and includes those in all years of Family Medicine, specialty or subspecialty training. "Program Director" means the person responsible for the organization of the individual training programs for the residents or fellows. "Resident" means a physician registered in a training program under the auspices of the Royal College of Physicians and Surgeons of Canada (RCPSC) or the College of Family Physicians of Canada (CFPC). "Fellow" means a physician registered in a training program, approved by the Faculty of Medicine, UBC, for advanced training and not receiving credit for a program recognized by the RCPSC or CFPC. "Dean" means the Dean of the Faculty of Medicine, University of British Columbia. "Associate Dean" means the Associate Dean of Residency Training, Faculty of Medicine, University of British Columbia. "PAR-BC" means the Professional Association of Residents of British Columbia, a recognized trade union in the province of British Columbia. "Collective agreement" means the current collective agreement between PAR-BC and Health Employees Association of British Columbia (HEA-BC), an association representing the hospitals who employ resident staff; or any other legal agreement between the resident staff and hospitals. "College" means the College of Physicians and Surgeons of British Columbia, the licensing body for physicians in B.C. "University" means the University of British Columbia. "Training Committee" means the committee responsible to the Program Director for organizing the training program. I. STATUS OF RESIDENT STAFF 1. Employee Resident staff are employees of the "hospitals" and, as members of PAR-BC, have a collective agreement with the HEA-BC or other hospitals; 2. Physician All resident staff hold a licence from the College and, as with all other physicians, the College is responsible for maintaining standards of licensure. Complaints to the College can be made by any member of the public, or any physician, but are largely confined to three areas: 3. Trainee Resident staff are registered at the University of British Columbia, and have the academic portions of their training under the auspices of UBC. In addition, residents are registered as trainees with the RCPSC or the CFPC. II. DISMISSAL OF A RESIDENT FROM A TRAINING PROGRAM A resident staff's position and progress in their academic program are dependent upon their maintaining satisfactory status as an employee, as a licensed physician, and as a trainee under the University guidelines. Dismissal from a training program by the University may result from one of three reasons. a) Dismissal by the University b) Dismissal as an Employee by a Hospital c) Loss of Licensure with the College III. IDENTIFICATION OF WEAKNESSES In the first instance, it is the responsibility of the Program Director to bring any academic weakness or other problem to the attention of the resident staff and to suggest and arrange remediation, if appropriate. Notice of weakness, along with the suggested remediation and a specified time during which improvement is expected, should be given to the resident staff in writing and should be signed by the resident staff, thereby acknowledging receipt of the notice. IV. REMEDIATION This is a defined period of time with the training components structured to address areas of weakness identified by the program director. It includes special evaluations which may be of more than one kind, and may be performed by multiple internal or external evaluators. The evaluations should be discussed with the resident staff, and signed by the resident staff, evaluator(s) and the program director. V. PROBATION After having received a notice of weakness and been provided with remedial training, the resident staff is expected to have improved his/her performance in the identified area. At the end of the specified time, the resident staff should either be notified that the weakness has now been corrected or, alternately, informed that the weakness still exists and that the Program Director intends to place them on probation. If the resident staff is to be placed on probation, a meeting must be held with the Head of the Department or Hospital, the Program Director, one or more members of the training committee, and the resident staff in question. The resident staff may choose to have at this meeting: a) a resident staff representing PAR-BC, At the meeting, the resident staff with the identified weakness should be informed of the following in writing: The resident staff should acknowledge receipt of this document by signing it. The proceedings of this meeting should be fully documented and a record kept in the office of the Program Director. The probationary period is a defined period of time, structured to address areas of weakness previously defined and evaluated in the remediation period. It includes special evaluations which may be of more than one kind, and may be performed by multiple internal or external evaluators. The evaluations should be discussed with the resident staff, and signed by the resident staff, evaluator(s) and the program director. At the end of the probationary period, the above named Committee must meet again and discuss with the resident staff his or her progress. The resident staff will either be: VI. IMMEDIATE DISMISSAL - "UNSUITABILITY FOR THE PROGRAM" The preceding paragraphs document the usual procedures that will take place when the issue of a resident staff's weakness is primarily of an academic nature. There will be instances, however, in which the resident staff is deemed by the Program Director to be "unsuitable" for reasons which are beyond remediation. Such factors may be the lack of a basic skill such as physical dexterity in the case of a surgical specialty, the presence of personality problems related to the trainee's ability to perform, unprofessional conduct, or other qualities of the resident staff which make them unsuitable. Decisions involving "unsuitability" are made by the Program Director, but must be approved by Head of the Department prior to any action being taken. The Associate Dean must be informed, in writing, of such decisions. VII. DISMISSAL If, by using either of the above two mechanisms, (V or VI), a decision is made to dismiss the resident staff, the hospital as employer will terminate the contract of a resident staff if advised by the Program Director that the resident staff is "unsuitable". This can be done formally through the contract under Article 6 "Termination - Unsuitability for the Program". It should be noted that resident staff dismissed under Article 6 are entitled to either two month's remuneration or two month's notice of their dismissal. The resident staff will be given a copy of the Appeals document at the same time as they receive the notice of dismissal. VIII. APPEALS A) EVALUATION a) the appeal must be made, in writing, to the program director In most cases, the Program Director and/or the Resident Training Committee will determine whether the appropriate process for an evaluation had been followed. The Committee may want to involve the Associate Dean - Equity as an independent arbitrator. If the appeal is successful, a new evaluation must be performed, which will be signed by the resident staff and placed in his/her file. The appealed evaluation will be removed from the file and destroyed. If the appeal is denied, the evaluation will be judged appropriate and valid, and will be placed in the resident staff's file. B) DISMISSAL The Faculty of Medicine Residency Training Committee, under the direction of the Associate Dean, shall maintain an up-to-date written appeals policy. Appeals will be held by the "Resident Staff Appeals Committee" as outlined under Article 6.03 of the contract. The resident staff who wishes to appeal a dismissal notice must give written notice of intention to appeal to the Associate Dean within ten (10) days. Within ten (10) days of submitting the Intention to Appeal, the resident staff should submit in writing the following: a) Statement of the decision which is being appealed; In most cases, within five (5) days of the receipt of this material, the Associate Dean shall inform the Program Director of this appeal and provide the Program Director with the material as supplied by the resident staff. Within ten (10) days the Program Director must submit to the Associate Dean: Within five (5) days, the Associate Dean will distribute all the material from the Program Director to the resident staff. Within seven (7) days of the receipt of the material from the Program Director, the Associate Dean will set a date for the hearing, usually within fourteen (14) days. The materials from the resident staff and from the Program Director will be distributed to the Resident Staff Appeals Committee at least seven (7) days prior to the hearing. It should be noted that all time frames in this document are approximate and may be altered at the discretion of the Associate Dean. IX. COMPOSITION OF THE RESIDENT STAFF APPEALS COMMITTEE 1. The Chair shall be the Associate Dean or an alternate appointed by the Dean. X. TERMS OF REFERENCE OF THE RESIDENT STAFF APPEALS COMMITTEE In the case of an academic weakness which has required remediation, the Committee shall determine whether the procedures set out above have been adhered to in determining the dismissal that the resident staff is appealing. There must be documentation to support this and there must be written evidence, whether from using regular Internal Training Evaluation Ratings or other forms of evaluation that the resident staff's progress has been fully evaluated. The Committee will confine itself to questions of "due process". As a general principle, the Committee cannot overturn academic judgement unless it is manifestly unreasonable. Where appropriate, the Committee may broaden its deliberations to ensure that the academic judgements made by the Program Director or other faculty members are both sound and fair. In the case of a resident staff deemed "unsuitable" for other than academic reasons, the Committee must satisfy itself that the reasons are both sound and fair. If appropriate, the Chair of the Committee will be empowered to seek a legal opinion on any matters arising out of the deliberations of the Committee. XI. PROCEDURES AT THE HEARING The following persons shall be present at the hearing: Prior to the actual meeting, all members of the Committee shall have copies of the written submissions of both the resident staff and the Program Director. At the hearing, subject to the rule of the chair, the following procedure shall be followed: Any member of the Committee may question either the resident staff, Program Director, or any witnesses present. The Committee may further request that it be provided with additional information other than that initially supplied. If such additional information is requested, both the Program Director and the resident staff must have an opportunity to read and respond to any submissions before a final decision is made. The Committee may adjourn and reconvene at the call of the Chair for these purposes. XII. DECISION The Committee shall arrive at a decision of the basis of a simple majority vote. (As noted in the Collective Agreement under Article 6.03). "The decision of the Committee will be final and binding." The decision of the Committee shall be communicated in writing to the resident staff, the Program Director and the Dean of the Faculty of Medicine within ten (10) days of the final hearing of the appeal. In its submission, the Committee shall give reasons for its decision. If, in the case of academic weakness, the Committee finds that due process has not been followed, or, if appropriate, that the academic judgement of the Program Director or other faculty members is not both sound and fair, the Committee shall recommend an additional specified period of training for the resident staff. The department or hospital will be obliged to reinstate the resident or intern for this period of time to ensure that any perceived weaknesses are re-identified and that due process is followed in bringing these weaknesses to the attention of the resident staff. The department or hospital will also be obliged to provide appropriate remediation. If there has been some procedural deficiency of a minor nature identified, but the Committee is satisfied that this procedural error could not have resulted in a wrong decision, the appeal may be disallowed. If the Committee finds that due process has been followed, and if appropriate, that the evaluations have been both sound and fair, or that it has been established that, for other reasons, the resident staff is "unsuitable", the decision of the Program Director will be upheld and the resident staff will be dismissed from the training program. If a resident staff is dismissed from the program, written confirmation of this decision should be sent to the RCPSC or CFPC as soon as possible. The Program Director may wish, or may be directed by the Committee to make a ruling on the eligibility of the resident's training for the purpose of credentialing whether the appeal on dismissal is upheld or dismissed. If the resident wishes to appeal this decision, he or she must address this appeal to the Committee. The Committee will follow the procedures as described under XI. and will either uphold or dismiss this appeal. A resident staff, registered at the University of British Columbia, has the privilege and right of appealing to the Senate. The procedure for this appeal is contained in the document "Policies and Procedures for Senate Appeals on Academic Standing". Copies of this document shall be kept in the Associate Dean's office and supplied to any member of the resident staff on request. Decisions regarding training evaluation for purposes of credentialing shall be transmitted in writing to the RCPSC, the CFPC, or other bodies as appropriate. Clinical Fellows Subspecialty Residents
Mindy Hundal
MHundal@cw.bc.ca
Adult ICU rotation goals and objectives
Pediatric anesthesia rotation goals and objectives
Pediatric cardiac anesthesia rotation goals and objectives
Pediatric cardiology rotation goals and objectives
Pediatric infectious diseases rotation goals and objectives
Neonatology rotation goals and objectives
Trauma rotation goals and objectives
APPEALS
a) General conduct;
b) Mental condition; and
c) Capability or fitness to the practice of medicine;
Most concerns about resident staff relate to their academic roles, and as such, this responsibility falls under the auspices of the University Faculty of Medicine and the Associate Dean. Trainees in either a RCPSC or CFPC training program, residents are routinely evaluated, both formally and informally, as per the guidelines of the RCPSC or CFPC.
Resident staff can be dismissed by their employer, the hospital, for "just cause". The mechanism for this dismissal is described in Article 5 of the Collective Agreement.
All resident staff are either on the full or temporary register of the College. The College could entertain complaints against resident staff and after appropriate investigation, remove their license to practice. These mechanisms are outlined in the Medical Practitioners Act (Consolidated January 11, 1988).
b) another resident staff, not officially representing PAR-BC,
c) no other resident staff member.
a) That he or she is being placed on probation for a specified period of time;
b) The weaknesses which need to be corrected; and
c) The specifics of the second remediation (probation) program.
1) fully reinstated; or
2) be dismissed.
The resident staff may choose to appeal the process, including factual errors, of an evaluation. In this case,
b) the appeal must document the perceived error in process
An appeal of a notice of dismissal must be made to the Dean of the Faculty of Medicine using the following guidelines:
b) The basis of the appeal;
c) Copies of documents or supporting evidence which the resident staff wishes to submit; and
d) The names of any witnesses that the resident staff will call at the hearing.
a) A confirmation of the decision which the resident staff is appealing;
b) The Program Director's response to the substance of the resident staff's appeal;
c) Copies of any documents or information which supports the decision taken by the Program Director; and
d) The names of any witnesses the Program Director will call at a hearing.
2. A Program Director from another department or hospital, appointed by the Associate Dean; and
3. A PAR-BC representative, jointly selected by the resident staff and the Associate Dean.
a) All members of the Resident Staff Appeals Committee;
b) The resident staff making the appeal;
c) The Program Director from the Department or hospital in question;
d) Any witnesses who will be called by the resident staff, the Program Director, or the Committee.
a) The Program Director may make an opening statement;
b) The Program Director may call and examine any witnesses;
c) The resident staff may cross-examine the Program Director or any witnesses so called;
d) The resident staff may make an opening statement;
e) The resident staff may call and examine such witnesses as he or she sees fit;
f) The Program Director may cross-examine the resident staff or any of the witnesses so called.
g) The Program Director may make a closing statement;
h) The resident staff may make a closing statement; and
i) Any members of the Committee may, through the Chair, question any witness, the Program Director, or the resident staff, at any time.
XIII. TRAINING EVALUATION FOR PURPOSES OF CREDENTIALING
Dr. Monika Sharma
Dr. Ashraf Znait
Dr. Uche Anene-Nzelu
Dr. Mikhail Barday (Lead Fellow 2024-25)
Dr. Hafsa Alsharif
Dr. Mohammed Alkathimi
Dr. Andrea Van Ransbeeck
Dr. Kaitlyn Lopushinsky
Dr. Lyndsay Greasley